- Facet joint Radiofrequency Thermocoagulation (RFT) Treatment
- Radiofrequency Thermocoagulation Dorsal root ganglion (DRG) radiofrequency thermocoagulation (RFT)
- Discitis Procedure
- Sacroiliac Joint Radiofrequency Treatment (Simplicity)
- In-Disc Ozone Therapy
- Nucleoplasty
- Transforaminal Injection (Pinpoint)
- Facet joint block
- Epidural Injection
Vascular Port (Permanent Vascular Access)
- Home
- Vascular Port (Permanent Vascular Access)
- Vascular Port (Permanent Vascular Access)
Contents
Toggle- Creating an individualised treatment plan
- The role of different specialities (physiotherapist, orthopaedist, psychologist, neurosurgeon)
- Pain treatment during pregnancy
- Treatment of chronic pain in the elderly
- Pain management in children
- Stress management
- Healthy eating
- Ergonomic living arrangements
- Exercise and mobility
- Facet joint Radiofrequency Thermocoagulation (RFT) Treatment
- Radiofrequency Thermocoagulation Dorsal root ganglion (DRG) radiofrequency thermocoagulation (RFT)
- Discitis Procedure
- Sacroiliac Joint Radiofrequency Treatment (Simplicity)
- In-Disc Ozone Therapy
- Nucleoplasty
- Transforaminal Injection (Pinpoint)
- Facet joint block
- Epidural Injection
- Cancer pain
- Permanent Epidural / Spinal Port Application
- Vascular Port (Permanent Vascular Access)
- Trigeminal Nerve RFT
- Blockade of Ganglion Stellatum
- Lumbar Sympathetic Ablation
- Facet joint Radiofrequency Thermocoagulation (RFT) Treatment
- Radiofrequency Thermocoagulation Dorsal root ganglion (DRG) radiofrequency thermocoagulation (RFT)
- Hernia Burning (IDET)
- Discitis Procedure
- Sacroiliac Joint Radiofrequency Treatment (Simplicity)
- Permanent Epidural / Spinal Port - Pump System
- In-Disc Ozone Therapy
- Nucleoplasty
- Peripheral Nerve Block
- Transforaminal Injection (Pinpoint)
- Facet joint block
- Epidural Injection
- Intra-articular Fluid Treatment
- Dorsal root ganglion (DRG) radiofrequency thermocoagulation (RFT)
- Spinal cord stimulation (pain pacemaker)
- Ergonomic living arrangements
- Spinal cord stimulation (pain pacemaker)
- Nucleoplasty
- Radiofrequency ablation
- Herbal solutions
- Dry needle treatment
- Anti-ageing treatments
- Ozone therapy
- Cupping therapy - Cupping
- Mesotherapy
- Prolotherapy
- Acupuncture
- Stem Cell Therapy
- Nerve blockages
- Corticosteroid injections
- Massage and relaxation techniques
- Manual therapy
- Electrotherapy
- Neuropathic pain medications
- Anti-inflammatory drugs
- Muscle relaxants
- Painkillers (paracetamol, ibuprofen, etc.)
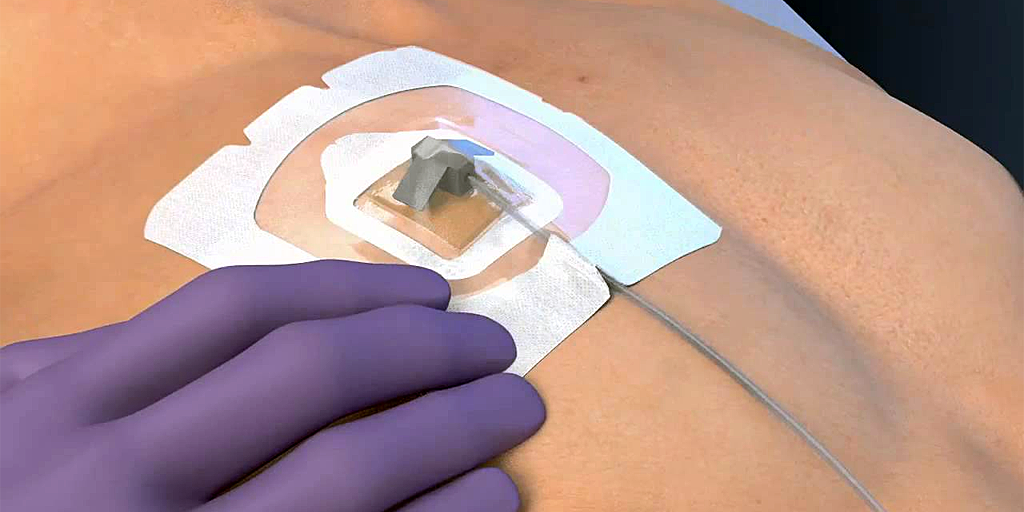
WHAT IS A VASCULAR PORT?
A vascular port is a medical device placed under the skin that is used in patients who require long-term intravenous administration of medication or fluids. The port is connected via a catheter (thin tube) to a large vein (usually one of the main veins in the upper chest area) and has a "reservoir" (port chamber) at the top, under the skin. This makes it easily accessible from the outside, but because it is hidden under the skin, there is less risk of infection and blockage.
The most common uses of the vascular port system are the administration of chemotherapy drugs to patients undergoing cancer treatment, blood diseases requiring frequent blood transfusions and chronic diseases that are difficult to establish a vascular access. The port makes the procedures more comfortable and reduces the need to search for a new vascular access each time.
WHY IS A VASCULAR PORT PREFERRED?
- Long Term Treatments:
In cases such as cancer, chronic blood diseases or long-term intravenous antibiotic therapy, the need for frequent intravenous access arises. Port saves these procedures the trouble of repeated venipuncture. - Vascular access difficulties:
Due to continuous needle interventions, the veins in the arms can become weak, narrowed or tender. The vascular port provides direct access to the veins via a single entry point. - Lower Risk of Infection:
Since the port system is placed under the skin, it is not in constant contact with the external environment. This reduces the risk of catheter-related infection in the long term. - Patient Comfort and Quality of Life:
Patients can continue their daily activities (shower, light exercise, etc.) more comfortably because there is no continuous catheter or vascular access in the arms.
HOW IS THE VASCULAR PORT PLACED?
- Planning and Preparation:
- The patient's general state of health, blood values and coagulation functions are checked.
- The type of anaesthesia (usually local anaesthesia or sedation) is determined.
- Operation Phase:
- The surgeon or interventional radiologist makes a small incision (approximately 3-4 cm) in the upper chest area.
- The port chamber is placed under the skin. The catheter tip is advanced into a large vessel (usually the superior vena cava).
- To make sure that the catheter is in the correct position, scopy (live X-ray imaging) or ultrasound is usually used.
- Sewing and Control:
- The incision site is closed with a suture and the port is fixed under the skin.
- Finally, X-rays can be taken to confirm the correct position.
BENEFITS OF VASCULAR PORT
- Single Point Access: It increases the comfort of the patient in regular intravenous administrations and eliminates the necessity to constantly seek a new intravenous line.
- Long Lasting Use: With proper care and cleaning, it can operate smoothly for months or even years.
- Low Maintenance Requirement: Requires less dressing and processing than peripheral catheters.
- Daily Life Advantage: Since there is no catheter or tubing visible from the outside, it offers the opportunity to perform social and physical activities more freely.
VASCULAR PORT CARE
- Cleanliness and Hygiene:
- The skin in the port area is regularly cleaned with antiseptic solutions.
- In port use, flushing with special heparin or saline solutions before and after each procedure reduces the risk of blockage.
- Regular Checks:
- Dressings can be changed as often as directed by the doctor or nurse.
- Look for any signs of redness, swelling or pain in the port area, especially after chemotherapy, blood transfusions or high-volume fluid administration.
- Avoiding Technical Problems:
- It is necessary to ensure that the needle enters the port chamber at the correct angle. Incorrect angle or too much pressure may cause displacement of the port under the skin.
- It is important for the patient to receive training in applications that can be done at home.
RISKS OF VASCULAR PORT
- Infection:
- Although the risk of infection is low, it can be an entry point for bacteria because there is a foreign body under the skin.
- In case of symptoms such as redness, increased temperature, pain or discharge, medical attention should be sought immediately.
- Blockage
- In ports that are not used for a long time or whose maintenance is neglected, clots or drug residues may accumulate and the catheter may become blocked.
- Regular heparinisation (heparin flushing) reduces this risk.
- Catheter Tip Displacement (Malposition):
- Trauma, sudden movements or incorrect needle insertion can displace the catheter. This can make intravenous injections difficult or cause pain.
- Vascular Injury
- There is a low probability of damage to the vessel during port placement or in the following period.
- In case of unexpected bruising, swelling or pain in the chest area, consult a physician.
- Rare Complications:
- Events such as port breakage, catheter rupture or catheter advancement into the heart are very rare, but require urgent intervention.
FREQUENTLY ASKED QUESTIONS ABOUT VASCULAR PORT
- Is it painful to have a vascular port inserted?
- The procedure is usually performed under local anaesthesia or sedation. There may be a slight feeling of pressure or pulling, but severe pain is usually not expected.
- How long do I have to stay in hospital after the port is inserted?
- In most cases, you will be discharged on the same day or after one day. Depending on the situation, your doctor may recommend an additional observation period.
- Can I take a shower when I have a port?
- Yes, since the port is under the skin, it is usually possible to take a normal shower. However, in the first days after the procedure, the suture area should be protected and the recommendations of your physician should be followed.
- Can I do sports and exercise?
- Light activities usually do not cause problems, but always consult your doctor before weight lifting, swimming or contact sports. Sudden and intense movements may cause displacement of the port.
- How long can I use the port?
- With good care and regular check-ups, the port can be used for many years. When the treatment is finished or the port develops problems, it can be removed by a surgical procedure.
- Can I have an MRI or CT scan with a port?
- Most modern ports are made of MRI-compatible material. Nevertheless, it is important to inform your doctor about the characteristics of your port before imaging.
- Is there a high risk of infection with port insertion?
- The risk of infection is lower in ports compared to peripheral catheters. However, like any invasive intervention, there is no zero risk. This risk is minimised with proper care and hygiene.
SUMMARY
A vascular port (permanent vascular access) is a comfortable and safe solution for patients requiring long-term intravenous drug, fluid or blood transfusion. With proper care and regular check-ups, the risks of infection and blockage can be minimised. If your doctor has recommended port placement, be sure to get detailed information about its advantages, possible complications and care processes. This will make your treatment process more comfortable and safe.
Our treatments
- Home
- Vascular Port (Permanent Vascular Access)
- Vascular Port (Permanent Vascular Access)